Chronic Lyme Disease Coinfection - Ehrlichiosis and Cancer Implications

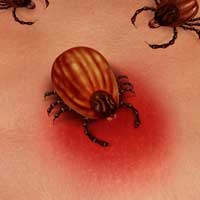
Patients who actually suffer from chronic Ehrlichiosis are often misdiagnosed as having autoimmune disorders or other chronic disease with similar symptomologies, as Ehrlichiosis is generally not tested for. Symptoms typically associated with this infection are a high fever, headache, chills, as well as muscular aches and pains. These closely mimic those often linked to other tick-borne diseases. The Lone Star tick (Amblyomma Americanum) bite is said to be the origin of HME, while HGE has been linked to the bites of both the Deer tick (Ixodes Scapularis) and the Western black legged tick (Ixodes Pacificus). The dog tick (Dermacentor Variabilis) is known to transmit both HME and HGE.
To make matters worse, Ehrlichiosis-transmitting ticks are also Lyme disease transmitters. For this reason, patients with Ehrlichiosis should also be tested for Lyme because the likelihood of coinfection is high, or at least worthy of testing.
Can It be Passed in a Blood Transfusion?
In parts of the Northeast, it is suspected that Lyme and many of its coinfections are found in great numbers in blood donors and as a result, transfusion supplies. With the demand for blood being what it is, it is not surprising that the time to test for Ehrlichiosis or other tick borne infections is passed over. Rather, supplies are tested for hepatitis and HIV but beyond that, little else.
In routine radiological studies of the central nervous system (CNS), analyses of cerebrospinal fluid (CSF) samples were seldom done. Only when primary care physicians detected specific symptoms or signs are such tests prompted to be performed. When they were, CSF samples were examined for 15 of 57 patients. 8 of those 15 were found to be abnormal. That is over 15 percent of the cases. The most common abnormalities were lymphocytic pleocytosis and elevated protein levels.
Chronic Lyme Disease and Ehrlichiosis - A Stealthy Infection with a Possible Cancer Connection
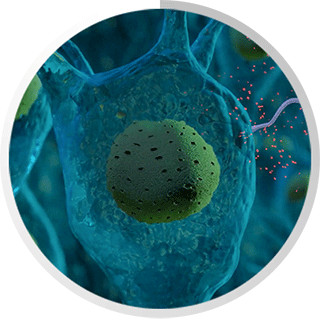
Ehrlichiosis is one of four bacteria known to survive and propagate within human neutrophils and their bone marrow progenitors. This tick-transmitted rickettsial pathogen, anaplasma phagocytophilum, is a causative agent of human granulocytic anaplasmosis and is found in the direct family line of Ehrlichiosis.
Neutrophils are the most abundant type of white blood cells (WBCs) in humans. In fact, about 70 percent of WBCs are of neutrophils. Intracellular bacteria do not consider them suitable hosts as they are short-lived and serve as primary defense cells that are armed with myriad antimicrobial apparatus.
A. phagocytophilum infection can alter neutrophil functions which can ultimately result in clinical disease. A. phagocytophilum infection can inhibit or retard processes such as apoptosis, oxidative burst and phagocytosis, while degranulation and cytokine/chemokine production are activated, leading to cancer in humans. No one is sure how many infections are cancer causatives, but this one may be recognized as a likely link to the idea that leukemia and other lymphatic cancers are catalyzed by epigenetic shifts resultant of Ehrlichiosis.
Ehrlichiosis and Immuno-Compromised Patients - A Recipe for Disaster
The zoonotic illness Ehrlichiosis is caused by Ehrlichia species. These bacteria are pleomorphic, intracellular, rickettsia-like organisms which present a clinical spectrum that can vary from a mild, influenza-like illness to a fulminant sepsis syndrome. In most cases, Ehrlichiosis is self-limiting and not fatal with death rates in large, unselected series ranging from 1 to 8 percent. This contrasts sharply with the high death rate in patients who are immunocompromised.
The Central Nervous System Invader
Up to 20 percent of Ehrlichiosis patients suffer neurologic manifestations including everything from confusion to frank meningitis. One patient battled obundation and delirium that persisted even after doxycycline therapy was administered and fever had dissipated.
Should headache and confusion come with pancytopenia and transaminase elevation, one must strongly consider an Ehrlichia infection, particularly if the patient has had potential tick exposures.
Nevertheless, an Ehrlichiosis diagnosis is typically delayed due to nonspecific clinical or lab manifestations. In those who are already immunocompromised, the search for an array often delayed because of its nonspecific clinical and laboratory manifestations. In the immunocompromised person, the search for opportunistic infections may further obscure the recognition that Ehrlichia is present. Empiric antimicrobial regimens that are often administered for suspected cryptogenic bacterial and fungal sepsis to immunocompromised subjects rarely include drugs effective against Ehrlichia.
Diagnosing Ehrlichiosis and Chronic Lyme Disease
For any patient with potential tick exposure in an endemic area who is suffering with fever, transaminase elevations, new-onset thrombocytopenia or leucopenia, an ehrlichiosis diagnosis should be considered. For those who could be categorized as immunocompromised, the clinical manifestations are far more severe and can include neurologic deterioration, multiorgan failure, and even a TTP-like illness. Moreover, the doxycycline therapy response could be delayed. The use of PCR for confirmatory diagnosis and early empiric therapy can be life-saving.
The Immune System Holds the Key to Coinfections and Chronic Lyme Disease
Without question, a host's best defense against rickettsial infection is its cellular immunity. Ehrlichia clearance from peripheral blood in patients with HGE comes from elevated levels of interferon gamma. A mouse model of Ehrliciosis showed that immunocompromised mice suffer with persistent infection, with most eventually succumbing to the disease. Cellular immunity, whether begotten of immunosuppressive therapies or underlying disease, can compromise recovery and result in more severe disease and oftentimes death.