Fibromyalgia Breakthrough - Treat The Causes, Not Just The Symptoms

Idiopathic disease is defined as one that develops without any apparent or known causes. That is the term used for fibromyalgia, autoimmune diseases, including lupus and chronic fatigue syndrome. While many of these diseases have recognizable signs and symptoms, the lack of causality haunts medical schools, doctors, practices and hospitals. The only ones benefiting from lifelong symptom treatments associated with chronic fatigue syndrome, lupus, autoimmune disease, or fibromyalgia are the pharmaceutical companies who sell billions in medication to treat them. A long list of pain medications, sleep-aids, anti-depressants, and anti-inflammatories are not sufficient because the diagnosis is incorrect. Instead, let's look at what the possible causes are to these diseases.
An Overview of Fibromyalgia Symptoms
A Conventional Scientific Overview of CFS (Chronic Fatigue Syndrome) and Fibromyalgia Causatives
Below, is a quick list of idiopathic disease causes — we will give a clinical review and explanation as to what takes place.
- Brain abnormalities
- Genetic factors (HPA) axis
- A hyper-reactive immune system
- Viral or other infectious agents like (Chronic Lyme disease Complex)
- Psychiatric or emotional conditions
Are Genetics to Blame?
Chronic Fatigue Syndrome and fibromyalgia have been linked with genes involved in the hypothalamic-pituitary-adrenal axis and the sympathetic nervous system. These genes regulate response to trauma, injury, and other stressful events. Our ten years of clinical experience shows that while such traumas could play a role in the etiology (the trigger to exhibiting symptoms) of the disease, they are unlikely the conditions' causes.
What is the Hypothalamic-Pituitary-Adrenal Axis (HPA)? Does Lyme Disease Play a Role?
HPA makes up a multi-set of direct influences and feedback interactions among the hypothalamus, the pituitary gland (a pea-shaped structure located below the hypothalamus), and the adrenal, also called "suprarenal," glands which are small, conical organs on top of the kidneys.
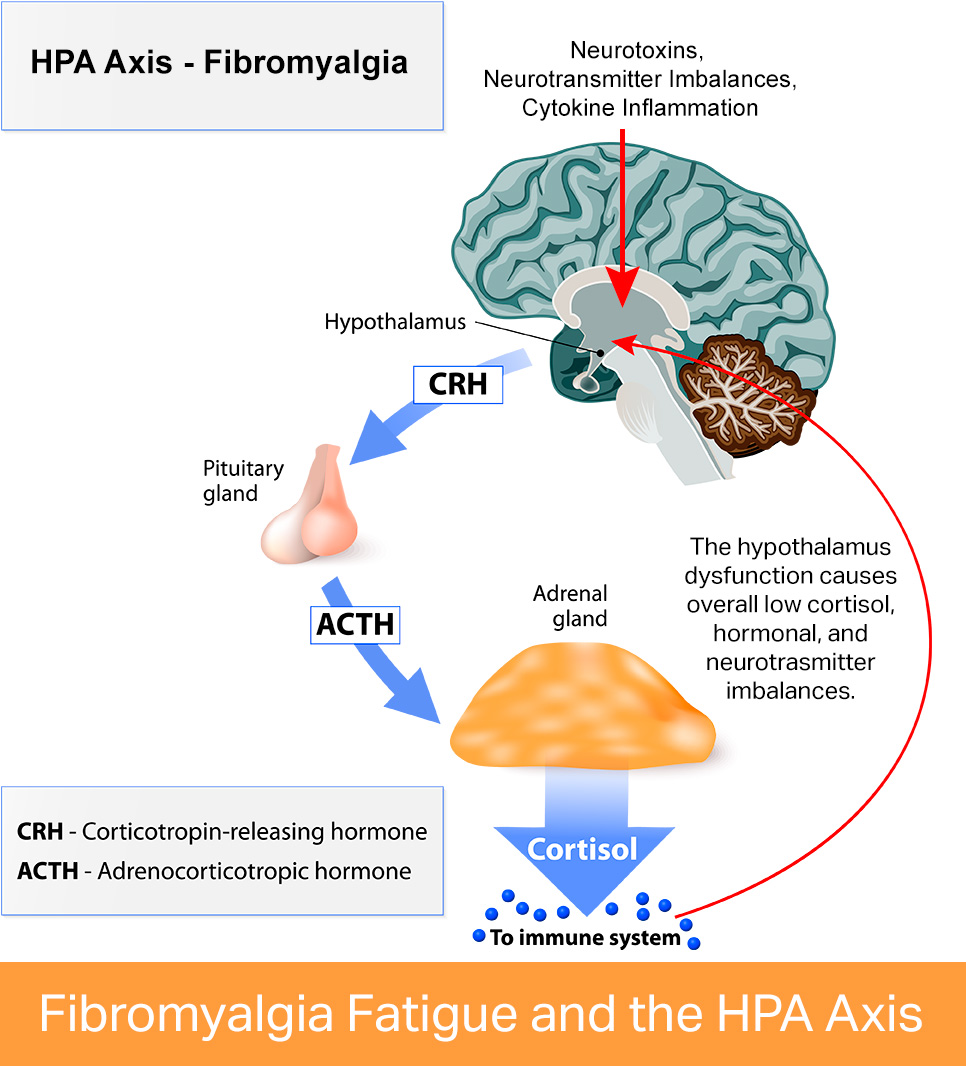
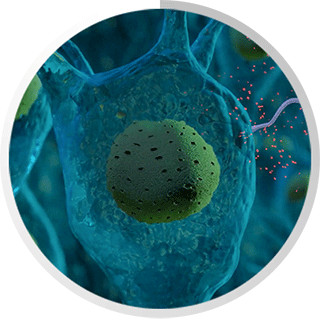
The interactions among these organs constitute the HPA-axis, a major part of the neuroendocrine system. From here, the body regulates reactions to stress, as well as processes such as digestion, the immune system, mood, emotions, sexuality, as well as energy. Infectious disease, such as chronic Lyme disease complex, impacts the HPA-axis via neurotoxins that compete for the same receptor sites used by the HPA-axis.
In fact, such infections can bring about identical symptoms of some idiopathic diseases listed above and many of the symptoms associated therewith. This should bring our attention to chronic Lyme Disease complex, which is composed of a number of infections and neurotoxins that bring about even more symptoms than those listed earlier in this article.
Does HPA Affect Fibromyalgia and Chronic Fatigue Syndrome?
Abnormal levels of certain chemicals regulated in the HPA axis area of the brain system have been proposed as a cause of Chronic Fatigue Syndrome and also have some influence in fibromyalgia. This system controls important functions, including sleep, stress response, and depression. Of particular interest to researchers are the chemicals and other factors listed below that are controlled by the HPA-axis.
The HPA-axis is involved in the neurobiology of mood disorders and functional illnesses, including anxiety disorder, bipolar disorder, insomnia, post-traumatic stress disorder, borderline personality disorder, ADHD, major depressive disorder, burnout, chronic fatigue syndrome, fibromyalgia, irritable bowel syndrome and alcoholism. Antidepressants, which are routinely prescribed for many of these illnesses, serve to regulate HPA-axis function. All of these conditions and their symptoms are commonly seen in chronic Lyme disease patients that contain a host of infections and neurotoxins that block serotonin receptors in the brain.
Can Chronic Lyme Disease Complex or Infectious Disease Affect HPA?
Patients may have contracted an infection at any point in their lifetime. However, the symptoms of chronic Lyme disease complex or its coinfections may remain unseen or dormant until the individual is weakened by a trauma or trigger. This could be anything from childbirth or a car accident to the death of a loved one, a divorce or even a vaccine, as seen among children with weakened immune systems.
In the etiology of chronic infectious disease, the traumatic event is a trigger, but not the cause of autoimmune disease, Chronic Fatigue Syndrome, or fibromyalgia. Nevertheless, treating these triggers is critically important to the new patient's care. What we find is that infection and not genetic defects are at the root of HPA-axis disruption in the brain itself.
The Major Impact of Epigenetic Changes
A number of studies have found that alterations in genes are caused by infections involving immune function, intracellular communication and energy transfer. Researchers have identified many different genes in patients with Chronic Fatigue Syndrome that relate to blood disease, immune system function, and infection.
However, despite these identifications, there is no clear pattern to them and it is quite possible that it is the infections alone that are altering these genes and are responsible for impacting mental and emotional health as well. It is very possible that the infections can alter these genes that impact mental and emotional health as well.
Important Neurotransmitters Changed by Neurotoxins Competing for Receptor Sites
Some patients with Chronic Fatigue Syndrome have abnormally high levels of serotonin, a neurotransmitter (chemical messenger in the brain), and also show deficiencies in dopamine, an important neurotransmitter associated with feelings of reward. In some cases there is also a demonstrable imbalance between norepinephrine and dopamine.
A number of studies on Chronic Fatigue Syndrome have shown patients have lower cortisol levels, a stress hormone produced by the adrenal glands. It has been suggested that such cortisol deficiencies are responsible for Chronic Fatigue Syndrome patients having impaired or weakened responses to psychological or physical stresses like worry, infection, or exercise. However, administering replacement cortisol improves symptoms only in some patients. Why? Infection and their toxins (neurotoxins) must be cleared before hormone replacement can begin to be effective in these patients. It is also common for these patients to have thyroid, testosterone and cortisol issues.
Idiopathic Diseases at Root of Myriad Psychological Disorders Including Sleep-Related Ailments
Evidence suggests that certain CFS, fibromyalgia, and autoimmune patients have disturbed circadian rhythms (disorder of the sleep-wake cycle), which is regulated by the so-called circadian clock, a nerve cluster in the HPA-axis. These are commonly seen in chronic Lyme disease complex along with a number of other neurological symptoms.
A mentally or physically stressful event, such as a viral infection, may disrupt natural circadian rhythms. An inability to reset these rhythms results in a perpetual cycle of sleep disturbances. Medications that improve sleep can be very helpful for certain patients with Chronic Fatigue Syndrome, fibromyalgia and autoimmune diseases. But, until the infections are cleared and hormones are rebalanced, long-term improvement is unlikely, as the patient is likely to relapse.
Psychological, personality and social factors are strongly associated with Chronic Fatigue Syndrome, fibromyalgia, and autoimmune disease like lupus. There is a distinct complex relationship between physical and emotional factors.
What Specific Infections are Responsible
Because most of the features of Chronic Fatigue Syndrome resemble those of a lingering viral illness, many researchers have focused on the possibility that a virus or some other infectious agent, in some cases, causes the syndrome.
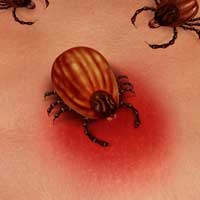
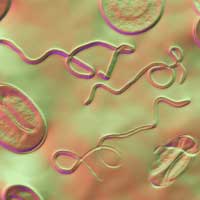
We have clinically determined that these patients usually have a group of viral, bacterial, parasitic and fungal infections that make up what we call Lyme Disease Complex. Some patients may or may not have actual Lyme disease but may have another type of tick-borne illness along with a host of co-infections that have brought about immunological, hormonal, and neuroendocrine changes.
Still, not all Chronic Fatigue Syndrome patients show signs of infection. And although experts have long been divided on whether infections play any role in this disorder at all, it does seem clear that subtypes of both viral and non-viral Chronic Fatigue Syndrome exist. That being said, researchers have seemingly overlooked the complexity of mute-infections, multi-toxins and heavy metal components that complicate these conditions, making them extremely difficult to diagnose on a case-to-case basis. When a complex of infections exists, they can affect the activation and replication of each other via biofilm communities. To be certain, most patients are never tested thoroughly and correctly for all the infections that make up chronic Lyme disease complex.
Infections Looking Like the Cause
The theory for Chronic Fatigue Syndrome having a viral cause is not based on hard evidence, rather, on an ever-growing series of observations. Chronic Fatigue Syndrome, as well as Fibromyalgia and Autoimmune disease patients, are often found with elevated levels of antibodies to many organisms that cause fatigue and other Chronic Fatigue Syndrome symptoms. Such organisms include those that cause Lyme disease, Candida ("yeast infection"), herpes virus type 6 (HHV-6), human T cell lymph tropic virus (HTLV), Epstein-Barr, measles, coxsackie B, cytomegalovirus, or parvovirus.
Many of these infectious agents are very common; however, none have emerged as a definitive cause of CFS. Well-designed studies of patients who met strict criteria for CFS without any known cause have not found an increased incidence of any specific infection(s).
In up to 80% of cases, CFS starts suddenly with a flu-like condition. In the U.S., there have been reports of cluster outbreaks of CFS occurring within the same household, workplace, and community (but most have not been confirmed by the Center for Disease Control and Prevention). However, most cases of CFS occur sporadically in individuals and do not appear to be contagious. These all have the pattern of infections and more importantly, complexes of infections taking over the patient's immune system, which is clearly seen in the depressed CD57 markers found in almost all of this population.
Infection Complexes Leading to Immune System Abnormalities and Immuno-Compromised States
CFS is sometimes referred to as "Chronic Fatigue Immune Dysfunction Syndrome." In many cases, studies have detected many immune system irregularities. Some components appear to be over-reactive, while others appear to be under-reactive, but no consistent picture has emerged to explain CFS as a disease of the immune system in conventional medical practices. Chronic Lyme disease patients almost always have depressed CD57 marker called the striker panel and this is almost never run on chronic fatigue patients when they go to their doctor. Almost 100% of the time we find decreased key immune function in all CFS patients because we are running the correct diagnostics.
Autoimmunity Overlaps with Other Conditions
The risk profile for CFS is similar to the risk profiles for a number of autoimmune diseases. Studies are inconsistent with regards to the presence of auto-antibodies (antibodies that attack the body's own tissues) in CFS, so the disease is unlikely to be due to auto-immunity, making it more likely connected to infectious disease. In Lyme disease patients, we typically see that the patient was diagnosed at one time or another with several autoimmune diseases, but almost certainly the previous physicians were confused. If you have any questions or would like to learn more about customized treatment options, contact us.