Understanding Lyme Disease

Lyme disease, also recognized as "the great imitator," is essentially one of the most misunderstood and widely growing illnesses in our country. Because its symptoms resemble that of so many other diseases and because our conventional medical community continues to be misinformed, stricken patients fail to receive the Lyme disease treatment necessary to restore their health. Because Lyme disease is so generally misinterpreted, standard treatment typically lasts only four to six weeks, with extensive treatment widely believed to be unwarranted.
As a result, many insurance companies refuse to cover appropriate treatment. Then, residual Borrelia reemerges, thus patients often relapse with Lyme or more specifically, Lyme Disease Complex. To further complicate matters, most patients diagnosed with Lyme disease are ignorant of the full "complex" of coinfections and neurotoxins that reside in their system – eliminating the possibility of prescription medication as a viable, singular Lyme disease treatment.
Results are not typical, and specific outcomes should not be expected. Envita Medical Centers does not guarantee outcomes. Treatment outcomes will vary per person to person based on that individual's personal and medical history. Always consult with your doctor before starting any treatment.
What is Lyme Disease Complex?
In the world of conventional medicine protocols, there is often lively debate regarding whether chronic Lyme disease is truly a bona fide disease. Others recognize that patients do indeed suffer from Lyme disease symptoms associated with Borrelia, which is contracted through tick bites.
Unfortunately, most care providers do not have knowledgeable LLMDs (Lyme Literate Medical Doctors) on staff who recognize the complexity, severity, and difficulty that encompasses Lyme disease treatment. To elicit a better understanding, the following are among the most common infections that can play a role in Lyme disease. They are all potential contributors to what we label Lyme disease complex – a confluence of infections that may simultaneously include bacterial, viral, parasitic, and fungal co-infections.
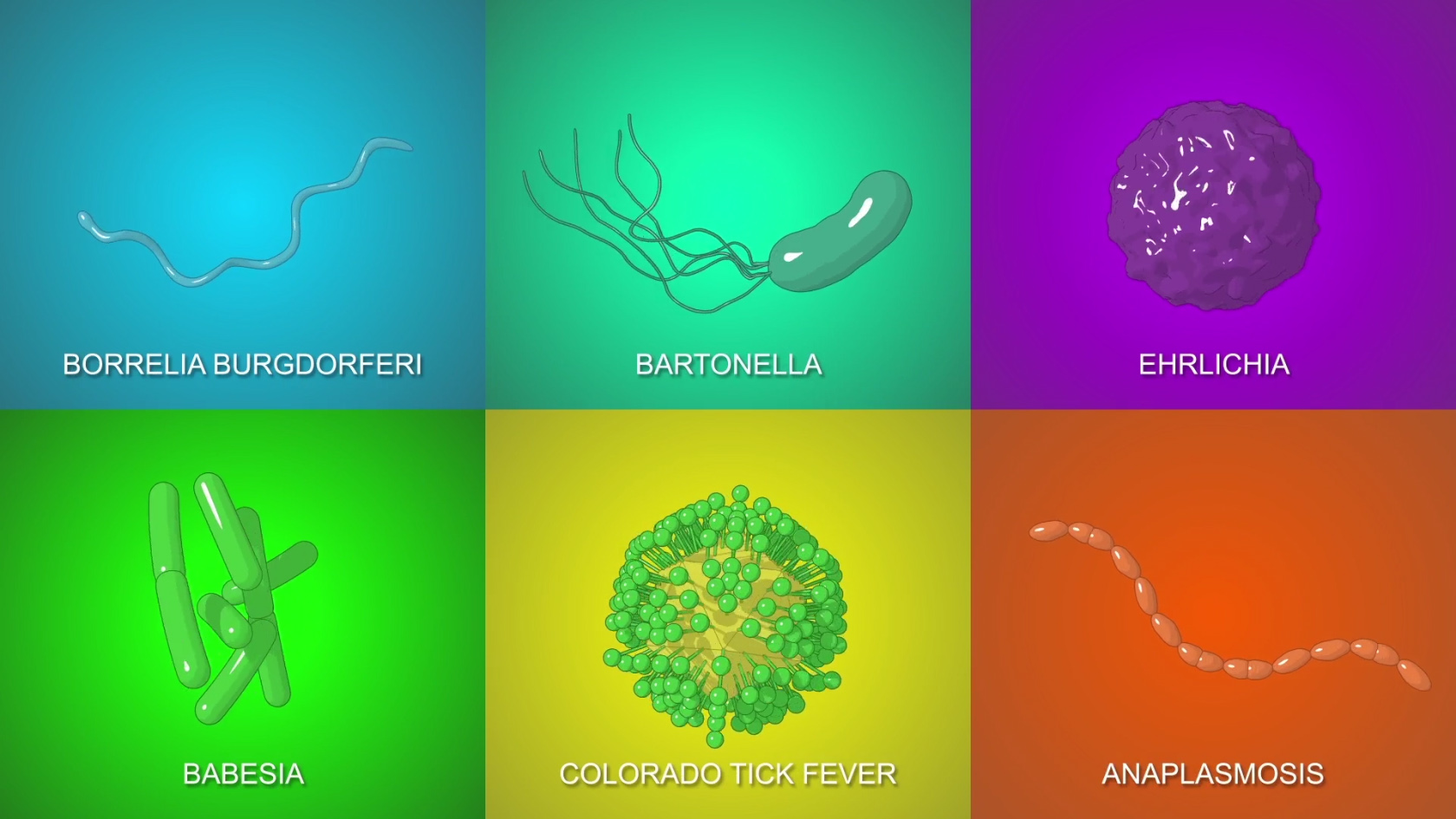
Borrelia (B. burgdorferi) - The most recognized infection in Lyme disease, which is often deemed to be the tick-borne variety. While it is a major contributor, borrelia alone makes up but one of the numerous infections that stimulate Lyme disease and ostensibly make treatment so difficult.
Bartonella - Bartonella henselae is the causative agent of the notorious cat-scratch fever, endocarditis, and countless other serious diseases known to humans. These bacteria comprise one of Lyme disease complex's most irksome co-infections. The bacteria are transferred by fleas, body lice, and ticks – with ticks being the greatest source of human bartonellosis infection, often accompanied by Lyme disease. Sand flies transport the bacteria in Peru's Andes Mountains, Colombia, and Ecuador while human body lice carriers are distributed throughout the world. The European sheep tick is a known carrier and five different species of Bartonella have been detected in nearly 20 percent of I. Pacificus ticks collected in California. Read more about Bartonella here.
Epstein-Barr (HHV-4) - This is a common human herpes virus that will infect virtually every individual on our planet at some juncture in their lifetime. It is indeed possible for EBV to lie dormant in the body throughout one's life span. Typically, the disease is transmitted via saliva and requires 30-45 days to present with symptoms, if it eventually does at all. During this time period, the host is most likely to spread EBV to others. However, when these infections continue to manifest as seen in chronic fatigue patients it becomes essential to evaluate or test for chronic Lyme disease complex, its coinfections and immunity. Lyme disease treatment becomes a requirement, as multiple infections can often awaken dormant insidious infections such as Epstein-Barr.
Cytomegalovirus (CMV) - Approximately 80 percent of adults in these United States are infected with cytomegalovirus (CMV). It is considered a member of the herpes family and shares the common trait of remaining alive, yet dormant, in the human body for the ongoing life span of its human host. Rarely does CMV become active unless the immune system is compromised– as it can easily be (and most often is) with Lyme disease infections deteriorating the immune system.
Babesiosis - Intraerythrocytic (occurring in red blood cells) parasite Babesia microiti causes Babesiosis, an infection that resides inside red blood cells. It is transmitted by the identical tick that transmits B. burgdorferi, the causative agent of Lyme disease. Forty-one percent of patients stricken with Babesia develop serious complications which may include acute respiratory failure, disseminated intravascular coagulation, congestive heart or renal failure.
Complex babesiosis is regularly associated with the presence of severe anemia and high parasitaemia levels. Chronic babesia has been known to trigger cardiovascular, kidney, and liver problems in patients. Babesiosis is clearly a dangerous component of Lyme disease and must be tested for, and if necessary, marginalized with a comprehensive Lyme disease treatment.
Human Herpes Virus 6 (HHV-6) - Lyme disease complex may also include human herpes virus 6. HHV-6 has since become one of the most widespread members of human herpes viruses and presents in two related variants: HHV-6A and HHV-6B. HHV-6 is known to attack specific cells including but not limited to CD 4 lymphocytes, NKTs, oligodedrocytes, CD8 cells, and microglial cells.
This virus is immune suppressive and also activates other viruses. While HHV-6 can remain latent for long periods of time, it can reactivate and produce infection quickly. A comprehensive Lyme disease treatment must be introduced to combat HHV-6 and other Lyme disease complex infections.
Ehrlichiosis - Ehrlichiosis is a serious Lyme disease co-infection disease caused by rickettsial-type (specific bacteria) organisms and presents in two specific forms; Human Monocytic Ehrlichiosis (HME) and Human Granulocytic Ehrlichiosis (HGE). In the majority of cases, Ehrlichiosis is self-limiting and not fatal with death rates in large, unselected series ranging from 1 to 8 percent [3,6-8]. This contrasts sharply with the high death rate in patients who are immunocompromised. Definitively, however, Lyme disease patients are relegated to the dangerous "immunocompromised" category. That is why it is incumbent upon patients to receive an aggressive and comprehensive Lyme disease treatment plan.
Chlamydia pneumonia - Chlamydophila pneumoniae (formerly known as Chlamydia pneumoniae or CP) are bacteria that infect humans and can trigger pneumonia, as they are a type of Chlamydia. Chlamydophila pneumoniae has a complex life cycle and must infect another cell in order to reproduce itself. The disease generally begins as a respiratory infection, appearing more or less unnoticed in the body and spreads to infect other tissues such as nerves, brain, muscles, blood vessels and even cells defending the body's own immune system, the macrophages.
CP itself produces at least two toxic substances that initiate tissue destruction and inflammatory burden, as well as a chronic immune activation and invasion with a toxin load. CP survives in the cell much as a parasite saps energy in order to reproduce. Therapy, however, must be administered effectively until CP is destroyed in all three stages, thus voiding re-infection. It is a critical part of Lyme disease treatment in cases where CP is present.
Candida - The most common organism implicated in fungal infections is the ubiquitous Candida, which is evidenced in the human digestive tract, mouth, and genital region (Eggiman P. et al 2003). Under normal circumstances, levels of Candida are controlled by beneficial bacteria. However, if the bacteria-fungus balance is skewed, by the use of antibiotics for example, or if the immune system is compromised, an overgrowth of Candida can occur, resulting in infection. As the immune system is always weakened by the presence of chronic Lyme disease complex, the presence of Candida must be aggressively addressed in a comprehensive Lyme disease treatment.
As comprehensive as the above maladies seem, it is equally important to point out that only 13% of infections that exist around the world have actually been identified. Among these are zoonotic infections (those emanating from animals), making Lyme disease treatment among the most complex to approach.
The Reality of Lyme Disease Treatments
If Lyme disease is detected early, it can be treated rather well with a realistic course of antibiotics. However, in a huge majority of cases, Lyme disease is not addressed by either the patients or their physicians at its onset, if they do at all. For patients who have had Lyme disease for more than a year, significantly more aggressive Lyme disease treatment must be authorized.
The standard prescription of antibiotics is categorically deemed insufficient when treating Lyme disease complex or as a sole Lyme disease treatment. Antibiotics do not help the body to destroy the mycotoxins or BLP (bacteria lipoprotein neurotoxins) caused by Borrelia, nor are they effective in treating the various viral, fungal, and parasitic co-infections attendant to Lyme disease. These coinfections are existent in some varied combination in virtually every Lyme disease patient and must be dealt with in any worthy Lyme disease treatment.
To be clear, is not uncommon to notice four or more combinations of infections in chronic Lyme disease patients. Often months, perhaps even years, of treatment are incumbent to remove the stubborn Borrelia from the body, not to mention the multitudes of other attackers liberated by the presence of Lyme disease complex in the body. Chronic Lyme disease treatment requires an organized/customized program that includes reestablishing immune function and status for patients. Simply administering medication will not be successful and can even further complicate matters.
Chronic Lyme Disease Awareness and Effective Treatments
Treatment of Lyme disease must be targeted at more than just the infections. Diminishing inflammation, supporting the immune system, detoxification of BLP's, and addressing hormone deficiencies are crucial to a comprehensive chronic Lyme disease treatment plan.
If patients are ingesting other medications or pain killers, a delicate approach is needed to transition them to a superior quality of life. In fact, when patients indicate that they have Lyme disease, or Lyme disease doctors examine patients, it is a commonly recognized that they are dealing with a combination of infections, as well as an immune compromised state. While the infections present may vary from case to case, the basic existing problem is Lyme disease complex or a combination of infections.
Our Experience Makes the Difference
We have worked in the field of Lyme disease research and Lyme disease treatment for over a decade. Our experiences have prompted more efficient, effective progress in Lyme disease treatment. We address and examine all factors of Lyme disease, assuming that handling Lyme's coinfections are just as critical as direct treatment of the primary disease. Understanding the concept of co-infections and body's homeostasis imbalances are the reason we refer to it as chronic Lyme disease complex.
To further complicate matters, many Lyme disease infections live within the red and white bloods cells making them very stealthy and extremely difficult to treat. They can deter the body's immune defenses and reproduce within the healthy cells. We take advantage of special shuttling agents to effectively address and treat these pervasive infections.
Treatment for Lyme Disease and the Possible Complications
There has been much dialogue about biofilm communities that protect the infections from the penetration of medications. In many cases these biofilm communities must be stripped and minimized through proper treatment and lifestyle changes.
Another scenario to consider, as it pertains to Lyme disease treatment, is self-synergistic replication. In this situation, many infections can communicate with and stimulate the replication of other viruses already present in the body. All the while, the patient must contend with numerous symptoms that may present as digestion problems, cognitive difficulties, chronic pain, sleep deprivation and hormonal imbalances, just to mention a few.
Does Chronic Lyme Disease Exist and is Treatment Really Necessary?
Lyme disease does undeniably exist. And even though many researchers will imply that the patient really does not have Lyme disease in the classical laboratory form, patients often still suffer from a combination of the infections aforementioned . Presumably, they must be treated simultaneously so as to provide effective and sustained relief for patients.
It is also vital to realize that many laboratory tests provide false negatives. The tests decree a negative finding when the patient actually has an infection(s) present. Some of the most common reasons are immune systems that are too compromised to mount a proper antigen test. However, if an immune system challenge is conducted, one may notice a positive test result for these patients. Additionally, many of these infections do live intracellularly and as a result return with false negative results.
We have developed a bold combination of tests to identify specific immunological factors and a comprehensive clinical overview to help patients seek and treat all the components of the Lyme Disease complex.
Our Approach
Because Lyme disease is so complex, extensive and comprehensive treatment is required. Lyme disease treatments are not limited to antibiotics, rather administered in conjunction with aggressive natural therapies from locations all over the world.
As part of our Disease Solutions Program®, we take an integrative approach to Lyme disease treatment, utilizing anti-viral, anti-parasitic and anti-fungal approaches, depending on the coinfections and symptoms present in each patient. By addressing every Lyme disease complex factor, we achieve superior results with our incomparable Lyme disease treatments.
We implement innovative treatments to help patients achieve an intensive-grasp of their disease, thereby providing them with the ability to conquer. Our comprehensive approach to treatment helps speed healing time, enhance quality of life, and minimize the recurrence of Lyme disease. To learn more about our Lyme disease treatment protocols or if you have any questions about Lyme disease itself, contact us today.