Stop Treating Lyme Disease and Treat the Complex

Treating Lyme disease comprehensively isn't as easy as it sounds. Our vast clinical experience uncovers why so many patients suffer needlessly and never reach best outcomes. With the huge underreported number of cases and despite a burgeoning growth in public awareness, Lyme disease for so many is still masked as fibromyalgia, chronic fatigue syndrome, chronic pain, depression or some other autoimmune disease. Chronic Lyme disease patients are often referred to as “attention seekers” by most doctors. It is important to note that Lyme disease can mimic over 360 diseases with over 300 genetic variations of Borrelia (Lyme disease). Our team has developed a special proprietary and successful approach that allows us to target all of the infections and factors involved.
After over a decade of working in the field and helping patients successfully, the answer lies in the key difference between Lyme disease and what we call Chronic Lyme disease complex. In most of the cases, we see unfortunate patients given the diagnosis of Lyme disease, who were prescribed antibiotics and attained very short term lived results with mild improvement to say the least. However, it's the only thing that helped them at all. Patients believe that if they have the infection and receive antibiotics, that it's game over. This is certainly not the case with Chronic Lyme disease!
Many conventional doctors will often miss the Lyme disease diagnosis all together due to not being well-informed on CDC's (Center of Disease and Control) failed testing criteria. Unlike many other infections, Lyme disease does not involve one straight forward lab test: in fact it involves a battery of tests to include genetic bands, immunity coupled with thorough medical history and confirmatory symptoms. Finally, when the diagnosis is made, antibiotics are almost always prescribed. The journal of Clinical Infectious disease published a study headed by Dr. Raphael B. Stricker that concluded that prolonged antibiotic therapy may be useful and justifiable in patients with persistent symptoms of Lyme disease and co-infections with tick-borne agents. However, another opposing study was conducted by Department of Neurology, University Medical Center at Stony Brook, Stony Brook, NY.
After receiving either 28 days of ceftriaxone (2 g per day) or placebo, the investigators found that there was a modest benefit with a lower fatigue score among those receiving ceftriaxone, although there was no change in the other end points, such as neurocognitive function or the CSF biomarker. Because of serious adverse effects, 4 (7%) of 55 patients were hospitalized with complications of intravenous therapy; study investigators concluded that parental antibiotic therapy could not be recommended, because the single subjective improved measure could not be justified against the considerable complication rate (2).
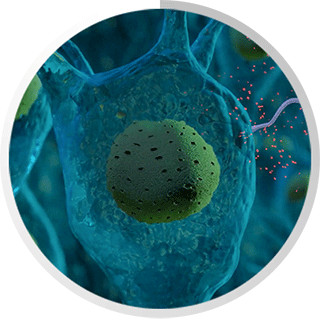
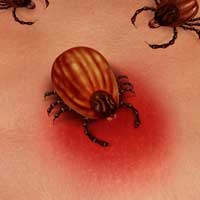
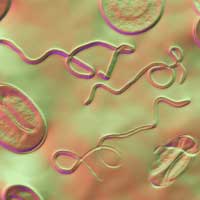
Taking into account that the antibiotic selections were different in the above studies, from a clinical perspective these outcomes are conflicting and confusing for patients. It all comes back to knowing the difference between “Lyme disease” and Chronic Lyme disease complex. Lyme disease in a vacuum is the infection of Borrelia (a spirochete that is most commonly transmitted by ticks). However, we define Chronic Lyme disease Complex or CLDC as: involving one or more factors: Lyme disease (as anchoring infection); its confection's; the reactivation of dormant infections, such as viruses, fungal and parasitic infections; and or an immune compromised state that can be further complicated by heavy metal toxicity, chemical toxicities, essential nutritional deficiencies and structural impairments as part of the etiology of the chronic disease. Lyme disease Complex presents itself as a multifaceted medical puzzle that cannot be simply solved with only oral or IV antibiotics alone. Point being, in a medical culture where it's difficult to find Lyme literate physicians that can treat you properly, it becomes almost impossible to find a doctor that treats this complex syndrome in an organized, comprehensive manner.
Our group has been working on solving this puzzle for many years. It starts with a proper diagnosis and treatment of all the infections involved: viral, fungal and parasitic co-infections that are often times more difficult to treat than the Lyme disease (Borrelia) itself. All these infections are connected and communicate with each other within your body; if one goes down the other up-regulates its replication until the vicious cycle is broken. Next, an in-depth functional medicine approach is implemented to correct all of the nutritional and amino acid imbalances while addressing old scar tissue, injuries and trauma that the body has suffered. Furthermore, selected medications are delivered in a proprietary method to cross the blood brain barrier and toxic metabolites removed from the central nervous system. This is all done while rebuilding immunity and restoring health. So many patients are confused when it comes to receiving treatment. When you don't treat Lyme disease complex you leave way too many health issues on the table that are unresolved for the patient; it's no wonder people don't get well! In the end, it's all about the personalized, integrative medical approach that works best for your individual case and getting the health you deserve. If you have any questions about Lyme disease or your current health condition, don't hesitate to contact us.